Rehabilitation for children and young people with Down syndrome

Mgr. Anita Herman
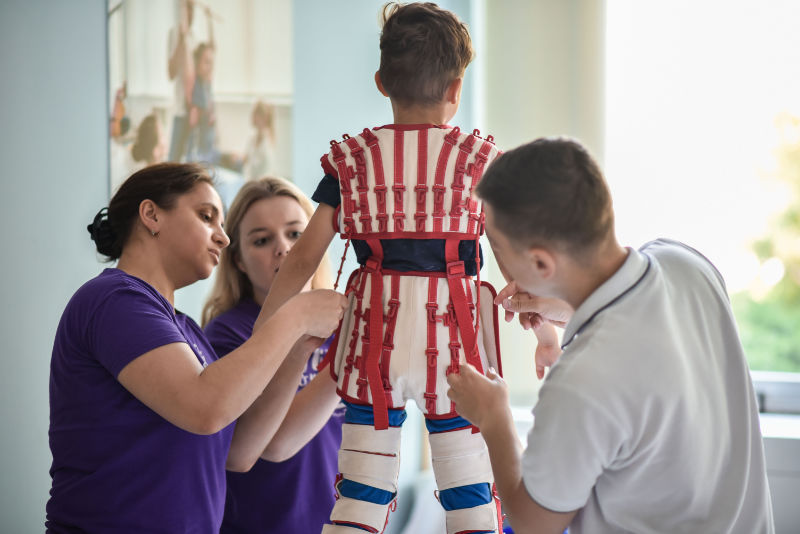
Intensive rehabilitation gives children and young people with Down syndrome and their parents the time and space to focus on their needs. While in the early years of life rehabilitation focuses on healthy motor and cognitive development, for adolescents the focus is on promoting their independence. For young children in particular, early rehabilitation can permanently improve their quality of life and naturally promote their social integration into society.
It is extremely important to create a motivating environment in which families are supported in developing the personality of children with Down syndrome by experienced professionals and the latest medical methods.
Your journey with us
Our multi-modal understanding of therapy means supporting motor skills and movement exercises, sensory awareness of your body, training fine motor and communication skills, speech understanding and expression, counseling with feeding issues or addressing other specific issues of a child or adolescent with Down syndrome.
Our goals for your child:
- Strengthening the musculoskeletal system
- supporting and improving movement skills
- osteopathic manual therapy
- Supporting communication skills and understanding
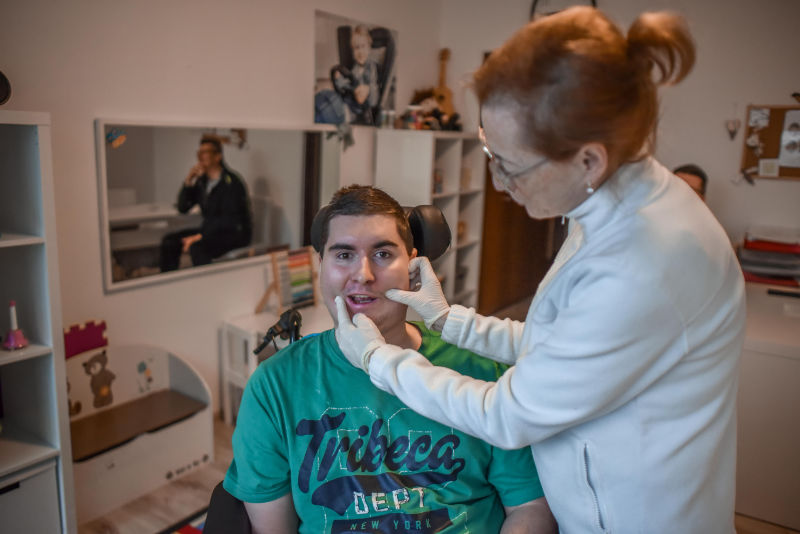
- Speech therapy stimulation of the face and oral cavity (chewing, swallowing)
- Supporting all-round personality development
- Training of hand-eye coordination, fine motor skills
- Improving memory and perception, cognitive abilities
- Practicing self-care activities in everyday tasks
- Improving social interaction with other people
- Developing and strengthening the competences